The Relation Between COVID-19 and Hypertension
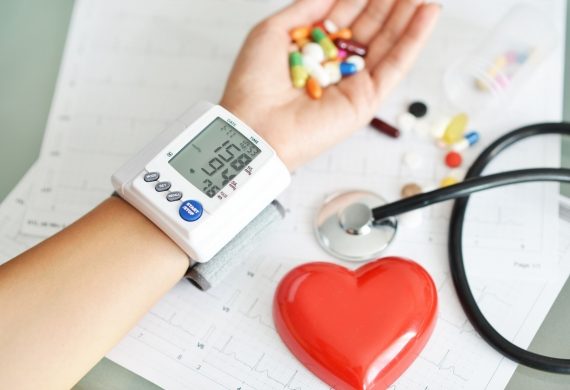
Hypertension is a common chronic disease in Singapore. Nearly 1 in 4 adult Singaporeans between the ages 39 to 60 has hypertension, and in the elderly age group of 60 to 69, the incidence of hypertension is as high as 50%. In fact, it is reported that about 20% of COVID-19 patients in Singapore have hypertension.
Are hypertension patients more susceptible to COVID-19? Why are there so many hypertension patients with COVID-19? Prof Tan Huay Cheem, Chairman of Singapore Heart Foundation and Director of the National University Heart Centre, Singapore; and Dr Mak Koon Hou, cardiologist and Assistant Honorary Secretary of Singapore Heart Foundation shares more about the relationship between COVID-19 and hypertension.
What is the relation between COVID-19 and hypertension?
Prof Tan: Since hypertension is a common chronic non-communicable risk factor, it is not surprising that it is also a common comorbidity among COVID-19 patients. This is particularly so when the more severely affected COVID-19 patients are the elderly.
The reported prevalence of hypertension among COVID-19 patients in a USA series was 56% compared to the Singapore and China cohorts, which stood at about 20%.
Hypertension can result in complications such as coronary artery disease, heart failure, chronic kidney failure, abnormal heart rhythms and stroke, which can worsen the general health and immunity of COVID-19 patients, especially among the elderly. The presence of such complications increases the morbidity and mortality risks of COVID-19 patients who also suffer from hypertension.
Dr Mak: A study done in Wuhan, China, concluded that the proportion of those with hypertension and severe disease was 24%. Conversely, it was only 14% for those with non-severe disease. This information suggested that patients with hypertension were more likely to succumb to a more serious form of COVID-19.
In addition, previous animal studies suggested that patients with certain blood pressure lowering medicines may increase an enzyme which is needed for the SAR-CoV-2 to enter the cells to cause disease. This finding gave rise to the hypothesis that those receiving these medicines were more susceptible to Covid-19.
However, the result of the clinical study did not consider other factors, such as age and diabetes, in their patients. As such, this association may be the result of the presence of these other factors instead of hypertension itself.
Although it is challenging to conduct a proper study to address this issue, recently, three observational studies provide sufficiently robust information that did not support this association. In New York University Langone Health system, the investigators did not find that patients with or without hypertension taking these medicines were more likely to have Covid-19 or suffer from a more severe form of the illness. Furthermore, one of these studies suggested that the risk of dying from Covid-19 was lower among patients taking one type of blood pressure lowering medicine which was previously thought to increase patient’s risk.
Does that mean that people with hypertension are more vulnerable to getting COVID-19?
Prof Tan: There is no reason to suggest that hypertension per se renders a person to be more susceptible to COVID-19 infection. Contrary to some of the previous reports, hypertensive patients who are taking a certain class of drugs known as angiotensin converting enzyme inhibitors (ACEI) and angiotensin receptor blockers (ARB) are also not more susceptible to contracting the virus infection. However, as the elderly are more likely to be hypertensive and age is also an important risk factor for COVID-19, it is not surprising the two diseases (hypertension and COVID-19) would occur concomitantly in many of these patients.
What causes blood pressure (BP) to spike?
Dr Mak: BP is the measure of the force required to pump blood throughout the body, delivering oxygen and nutrients to the body tissues and removing carbon dioxide and waste products. Therefore, it is not a constant reading and is affected by numerous factors such as stress (physical or mental) or physical activity.
Rather than maintain a “low” blood pressure, we should aim to maintain a “normal” reading. The risk for stroke, heart attack and kidney failure are related to high blood pressure. As the reading increases, the risk is greater. Several clinical trials have shown that normalising the blood pressure reduces the risk. However, there is likely to be a J-curve, in that, if the reading is too low, risk increases again. Therefore, it is important to maintain a normal blood pressure.
Prof Tan: Our BP is never a constant value. Blood pressure changes and fluctuations are a physiological response to any form of activities or stress (be it physical or mental). Physical stressors such as pain/discomfort and exercise will cause BP to be elevated. Likewise, emotional anxiety can also cause BP to rise. But these changes are transient and will resolve when the stress elements are resolved.
Certainly, when a patient is hospitalised with COVID-19 infection and is experiencing cough or breathlessness, he will have fluctuating BP. In managing sick COVID-19 patients, particularly in the ICU setting, BP becomes a key vital parameter. Maintaining BP stability will be a challenge in those patients with concurrent heart diseases or multiple comorbidities.
Why is it important to control our blood pressure?
Prof Tan: Controlling BP reduces the likelihood of an individual developing complications such as stroke, heart attack, heart failure, abnormal heart rhythms, kidney damage, blockage of the leg arteries, aortic dissection (‘tearing’ of large artery) and blindness. The medical and social burden brought upon by these complications is huge and parallels that of diabetes mellitus, for which Singapore is declaring a war against.
Blood pressure control can lower the risks of stroke by 40%, heart attack by 25% and heart failure by 50%.
What tips do you have for any hypertension patients, especially during this trying period?
Dr Mak: Apart from taking your prescribed medicines, it is important to watch your diet, especially your salt intake. Snacking and over-eating should be avoided, as weight increase is detrimental to blood pressure control.
Try adopting a suitable exercise regimen, but adequate rest is also essential for a healthy lifestyle.
Prof Tan: Besides staying compliant with the antihypertensive medicines prescribed by doctors, patients should continue to adopt a healthy lifestyle.
-
Choose a balanced diet
Choose a healthy and balanced diet that includes carbohydrate, protein, fruit and vegetables in meals, as they provide the necessary fuel for daily activities.
-
Reduce salt intake
Reduce your intake of salt, saturated fat and cholesterol, while increasing that of fibre and potassium, lean protein and high calcium from foods such as low-fat dairy.
The daily consumption of salt a day should be less than 5g (one teaspoon) as recommended by the World Health Organization. However, in the National Nutrition Survey 2020 conducted by Health Promotion Board (HPB), Singaporeans were found to consumer 8.3g daily.
Dietary salt occurs naturally in fresh food. It also comes from salt added in cooking, as well as preserved and processed food. -
Choose fresh food over preserved food
Choose fresh food over preserved food, look out for HPB healthier choice symbols such as “lower in sodium” or “no added sodium” and always reduce the use of additional salt and sauces in cooking or at the table. -
Exercise regularly
Regular physical activity is important.
The Ministry of Health’s recommendation is to aim for at least 150 minutes of moderate-intensity exercise a week, or at least 30 minutes of moderate-intensity exercise five to seven days a week.
-
Drink alcohol in moderation
Alcohol should be consumed in moderation. It adds to calorie intake and can cause weight gain.
The recommended amount is one can of beer, one glass of wine or one shot of hard liquor a day, and drinkers should keep at least two alcohol-free days a week.