Chest Pain: Am I Having A Heart Attack?
Chest pain represents one of the most frequent complaints in the Emergency Room and is also the hardest to assess. This is because a variety of cardiac and noncardiac conditions can produce chest discomfort or pain. History taking remains the most important technique for distinguishing among the many causes. A detailed description of the symptom complex enables the clinician to characterise the chest pain. 5 components are typically considered – quality, location, duration of pain, factors that provoke the pain and factors that relieve the pain.
Angina pectoris, or “heart pain”, may be a warning symptom prior to the onset of a heart attack. It is a form of chest discomfort which has been described as “choking” or “pressing”, “squeezing”, “strangling”, “constricting”, “bursting” or “burning” in character. Angina is most commonly felt in the midline of the chest but can manifest exclusively in the jaw or neck, the left shoulder or arm, especially in the ulnar aspect.
The typical patient is one who clenches his fist while describing the symptom, the so-called Levine sign. Angina is almost never sharp or stabbing, and it usually does not change with position or respiration. The anginal episode usually lasts for minutes.
A fleeting discomfort or a dull ache lasting for hours is rarely angina. It is generally caused by exertion or emotional stress and relieved by rest. The intensity of effort required to bring about the symptom seems to vary from day to day and throughout the day in the same patient. The anginal threshold is generally lower in the morning than at any other time of the day, thus activities that may cause angina in the morning might not do so later in the day. Rarely, the back interscapular region (between the shoulder blades) or right shoulder may be involved.
Typical angina is:
- Substernal (behind the breast bone) chest discomfort with a characteristic quality and duration
- Provoked by exertion or emotional stress
- Relieved by rest or nitrates (medicine taken under the tongue or in the form of a spray)
Atypical angina meets two of the above characteristics, while noncardiac chest pain meets one or none.
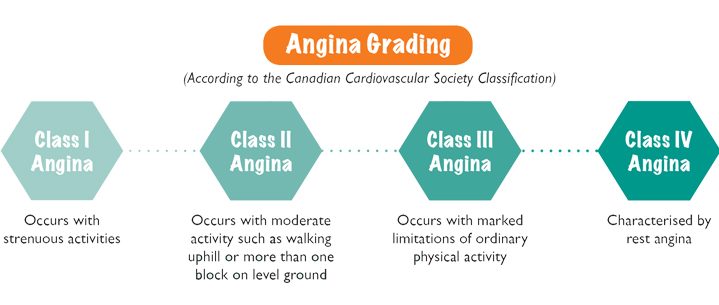
Angina is further classified as stable or unstable. Unstable angina is defined as angina that presents at rest, or as severe new-onset angina or increasing angina. It represents a state in which the patient is at a higher risk of developing acute coronary events such as acute myocardial infarction (heart attack) or death.
The pain from a heart attack is anginal pain amplified several folds. It is not relieved by rest and the patient frequently has associated symptoms of profuse cold sweat, nausea, vomiting, dizziness and shortness of breath. In severe cases, the patient may even lose consciousness completely from a cardiac arrest.
While angina pectoris is the most important cause of chest pain, it has to be distinguished from other causes too. The differential diagnoses or other causes include aortic dissection (or ‘tearing’ of the aortic wall), which may manifest as severe chest pain that radiates to the back and is migratory from its point of origin at the back down the spine, to other sites, following the path of the dissecting hematoma (or blood clot). The pain is maximal at its onset and may actually lessen in intensity with time, unlike heart attack pain which builds up in a crescendo pain after it begins.
Another common cause is acute pericarditis or ‘inflammation of the heart covering’. It is characterised by a precordial (front of the chest) pain that is preceded usually by a history of viral upper respiratory tract infection. It is sharper than anginal discomfort, typically left-sided, and is made worse by inhaling, turning in bed, swallowing or twisting the body. It may lessen when the patient sits up and leans forward. Chest wall pain of musculoskeletal origin is common in patients who are anxious about heart disease. Costochondritis or Tietze syndrome is characterised by focal chest wall pain and point tenderness (front of ribs), which is frequently aggravated by movement or coughing.
Emotional stress and anxiety precipitating functional or psychogenic pain (Da Costa syndrome or neurocirculatory asthenia) manifest as a dull, persistent ache below the left nipple that lasts for hours; and is punctuated by brief sharp stabs of 1-2 seconds duration. Esophageal discomfort from reflux esophagitis (‘heartburn’) may also mimic that of ischemic (anginal) heart pain. However, the symptom is usually brought on by food digestion and recumbency and the patient may experience a sour taste in the mouth.
Distinguishing chest pain arising from the heart with other causes may be difficult and it takes an experienced doctor to make an accurate diagnosis. The advice will be to seek immediate medical attention by calling for an ambulance service. Heart attack and some of the other causes may be easily diagnosed by performing a resting electrocardiogram for the patient.
Article contributed by Professor Tan Huay Cheem, the Chairman of the Singapore Heart Foundation’s Board of Directors. He is also the Director at the National University Heart Centre, Singapore (NUHCS).






