COVID-19 Infection and Heart Complications
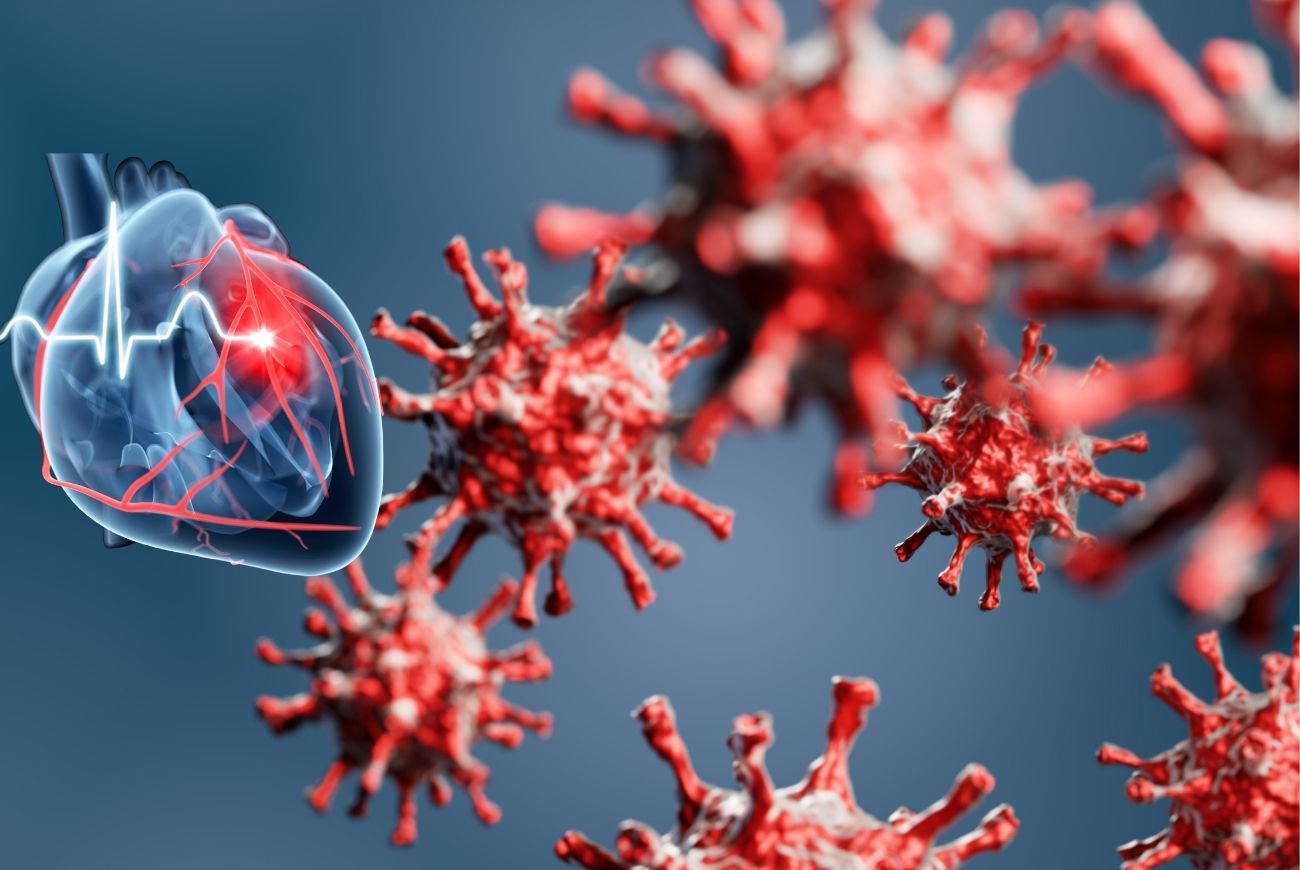
Whilst the COVID-19 virus primarily affects the airways and lungs, it is also well known that the ‘inflammatory storm’ that occurs during the infection can involve the heart, leading to multiple complications. Furthermore, any cardiac condition in an infected person seems to represent a major risk factor for an unfavourable outcome of the COVID-19 infection.
Studies have suggested that COVID-19 infection can cause myocardial (heart muscle) injury in 30% of infected individuals, as evident by an elevation of a blood biomarker known as troponin. The presence of elevated troponin levels indicates heart muscle damage which can arise because of multiple mechanisms such as inflammation (myocarditis), clot formation (thrombosis), which can lead to heart attacks, direct viral injury, heart failure etc. Cardiovascular complications are frequently seen in patients hospitalised with severe COVID-19 infection, and they are strongly associated with a higher risk of death. For the majority of the COVID-19 patients with a mild infection, the likelihood of cardiovascular complications is low.
Myocarditis, or inflammation of the heart muscles, in a COVID patient can occur without symptoms or can present in a catastrophic manner, such as in a state of cardiogenic shock. Fortunately, most patients with myocarditis, like in many other viral infections, have a self-limiting course and recover with no long term side effects. In the rare event of fulminant myocarditis, aggressive treatment will have to be instituted in the form of intravenous drugs to enhance heart contractility, ventilatory support, and even mechanical circulatory support such as extracorporeal membrane oxygenation (ECMO).
Heart attack is noted to increase by 3 to 8 times in the week after a COVID-19 diagnosis. The risk decreases steadily after that but remains elevated for at least a month. The trigger for this is likely the exaggerated inflammatory response that makes blood clot formation more likely. Patients with heart attack and COVID-19 infection have a higher risk of mortality at about 2.5 times that of non-infected patients. These COVID-19 patients are treated with emergency coronary angioplasty similar to other non-COVID patients.
Arrhythmias or abnormal heart rhythms have been detected in 20% of hospitalised COVID patients. The majority experience benign ventricular ectopy (‘extra beats’), which often does not cause symptoms, but may result in persisting palpitation, chest pain, dizziness and reduced quality of life in some patients. Rarely, serious arrhythmias like ventricular tachycardia may occur and require specific medicines or defibrillator implantation for treatment.
Heart failure can develop acutely as a complication of COVID-19 infection or as a worsening of a patient’s pre-existing impaired heart function. Patients who develop this complication have a higher risk of mortality. Most patients will recover their heart function if they survive the infection, but some may develop chronic heart failure.
Though the acute cardiovascular complications of COVID-19 infection are well known, the long-term effects on the heart are lesser-known. Some studies have suggested that survivors are still at increased risks for cardiovascular disorders such as heart failure, arrhythmias, clot disorders etc., even up to one year of the disease.
While heart patients may constitute a higher proportion of COVID patients with increased risks of acute and chronic cardiovascular complications, the risks remain low if pre-existing conditions are well managed and stabilised; and if they are fully vaccinated. However, should there be symptoms of chest pain, breathing difficulty, palpitations of prolonged duration, cold sweatiness or fainting spells, one should seek immediate medical attention. Heart disease patients who are elderly, frail with poor functional capacity, have multiple comorbidities and are unvaccinated remain the highest risk group for poor prognostic outcomes.
Article is contributed by Prof Tan Huay Cheem, Chairman, Singapore Heart Foundation, and Senior Consultant, Department of Cardiology, National University Heart Centre, Singapore.