Risk Factors
You can avoid heart disease or stroke by first being aware of the risk factors.
Factors you can change
This group of risk factors stems mainly from the personal habits and practices that we have cultivated since childhood. Although it is more effective to avoid developing unhealthy habits from young than to try and modify such habits later in life, the good news is that it is never too late to start adopting heart-healthy habits to reduce your risk of cardiovascular disease.
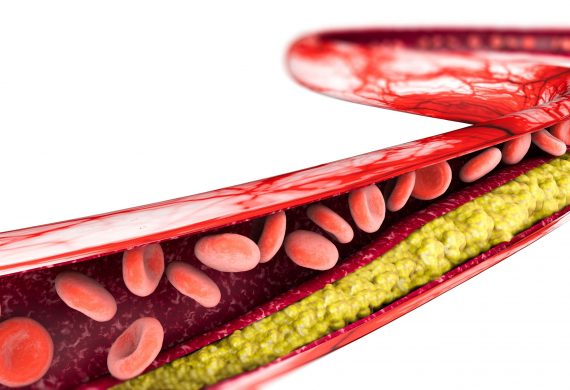
High Blood Cholesterol

Cholesterol, a fat-like substance, is produced naturally by our bodies and can become a problem when too much is in our blood. Cholesterol can build up with other substances in the inner walls of arteries and cause narrowing and hardening of blood vessels. The fatty deposits may also come loose and cause blood clots, resulting in a stroke or a heart attack.
The total cholesterol level in our bodies consists of both “good cholesterol” (HDL) and “bad cholesterol” (LDL). You need some fat in your diet, but too much fats, especially trans and saturated fats, may raise LDL (bad) cholesterol and increase your risk of heart disease. Your healthcare professional can measure your “good” and “bad” cholesterol levels through a blood test and tell you what the normal levels are.
If you need to lower your “bad” cholesterol and increase your “good” cholesterol, you can work with healthcare professionals to create a physical activity plan and a diet that is low in saturated fats and cholesterol.
Diet and exercise are important, but they may be insufficient. If these efforts do not enable you to achieve your goal, your doctor may prescribe medication. Even if you take medication, a healthy diet and regular exercise remain important.
Read more about the causes, symptoms and treatment for high blood cholesterol.
High Blood Pressure

High blood pressure or hypertension is often called a silent killer because it usually presents no symptoms. It forces your heart to work harder than usual, increasing the likelihood of causing injury to your heart. This raises your risk for heart attack and stroke.
The only way to know if you have this condition is to have a health professional check your blood pressure and monitor it using a home blood pressure machine.
Blood pressure measures the pressure of blood flowing through the blood vessels. It is recorded as two numbers, such as 120/80mmHg. Systolic pressure (the first number) is the pressure in the arteries when the heart contracts. Diastolic pressure is the pressure when the heart relaxes.
If your systolic pressure is 140mmHg or more, or your diastolic pressure is 90mmHg or more (or both) when measured on two or more occasions, you may be suffering from high blood pressure.
Read more about the causes, symptoms and treatment for high blood pressure.
Diabetes

Diabetes is a condition in which your body cannot regulate its sugar levels. This is due to a lack of a hormone called insulin. Diabetes is also associated with high blood pressure and high cholesterol.
There are two types of diabetes:
Type 1
Insulin-dependent Diabetes Mellitus (IDDM) – a condition in which insulin production is absent. This type of diabetes usually starts during childhood and is also referred to as “juvenile diabetes”. It is managed through regular insulin injections throughout their life.
Type 2
Non-insulin-dependent Diabetes Mellitus (NIDDM) – a condition in which the body still produces insulin but in insufficient amounts. The patient is usually treated with oral medications, either with or without insulin injections, diet modifications and physical activity.
If your fasting blood sugar level is relatively high (7 mmol/L or greater), please consult your doctor.
Read more about the causes, symptoms and treatment for diabetes.
Overweight / Obesity

If you have too much body fat, especially around the waist area, your risk of high blood pressure, high blood cholesterol, high triglycerides, diabetes, heart disease and stroke is higher.
The waist measurement and Body Mass Index (BMI) are commonly used to determine the risk of coronary artery disease. For Asians, a high-risk waistline is greater than 80cm for women and greater than 90cm for men.
BMI is a measure of body fat based on height and weight. Ideally, your Body Mass Index (BMI) should be within 18.5 – 22.9kg/m2. Singaporeans are at a greater risk of developing heart disease and diabetes when their BMI values are greater than 23 kg/m2.
Find out your BMI using our calculator.
Smoking

Smoking is one of the major risk factors for coronary heart disease. Carbon monoxide and nicotine in cigarette and cigar smoke deprive the body of oxygen. As a result, the heart has to work harder to supply oxygen to the body.
Nicotine also stimulates the heart, makes it beat faster and raises blood pressure. It promotes plaque deposits and increases the risk of clot formation in the blood vessels. Similarly, the carbon monoxide in cigarette smoke damages the inner lining of the blood vessels and may trigger the onset of atherosclerosis.
Other non-conventional smoking methods include the e-cigarette and shisha, which are often seen as “safer” options to tobacco smoking. However, this is not the case as both e-cigarettes and shishas contain nicotine. In fact, shisha smoke contains a high level of toxic compound, which exposes smokers to more carbon monoxide and toxic, as compared to cigarette smokers. Under the Tobacco Act, buying, using and possessing e-cigarettes and shisha are now illegal in Singapore.
Smokers face approximately three times the risk of having heart attacks than non-smokers. They are also more than twice as likely to have sudden cardiac death. Constant exposure to smoke exhaled by others increases your risk of coronary heart disease – even if you do not smoke.
The good news is that when you stop smoking – no matter how long or how much you have smoked – you will reduce your risk of heart disease significantly, as well as prevent the worsening of any existing cardiovascular (heart) conditions you may have. Your risk is reduced by half after one year without smoking and then continues to drop until it is as low as a non-smoker’s risk.
The first step is to plan to quit. Making a plan before you quit will increase your chances of success. Here are some tips for preparing to quit:
- Pick a date and tell friends and family
- Ask yourself questions such as “Who is my support?”
- Learn how to manage your withdrawal symptoms (symptoms which you may experience when you stop smoking)
- Symptoms vary between individuals, but may include dizziness, depression, headaches and sleep disturbances
- Decide how you are going to quit – cold turkey (just stopping) or gradually reducing the number of cigarettes you smoke, using nicotine replacement therapy (patches or gum), joining a tobacco cessation group, using self help materials or working with your local physician or counsellor.
- Think about changing your routine and avoiding situations and places that increase your urge to smoke
- Try to avoid passive smoking by spending your time in smoke-free areas
Physical Inactivity

Lack of exercise may double a person’s risk of developing and subsequently dying from cardiovascular disease. This is because a person who leads a sedentary lifestyle is more likely to become overweight and/or have high blood pressure, diabetes and high LDL cholesterol, increasing your total risk for heart disease and stroke.
You can change this by doing 150 minutes of moderate to vigorous-intensity physical activity per week. If you are new to exercise, find out how to start getting active safely.
Unhealthy Diet

According to the World Heart Federation, unhealthy diets are linked to four of the world’s top ten leading risk factors causing death: high blood pressure, high blood glucose, overweight and obesity and high cholesterol.
Diets high in sugars, saturated and trans fats; high intake of fast food, processed foods and high-sugar drinks; inadequate consumption of fruits and vegetables all contribute to heart health problems.
High dietary salt consumption also severely impacts blood pressure levels and overall cardiovascular risk. High blood pressure is the number one risk factor for death worldwide.
Find tips on healthy eating.
Stress

Stress is the psychological tension caused by physical, emotional, socio-economic, or mental pressure. It is a normal human response to keep us from pushing ourselves beyond our own limits.
Moderate amounts of stress may sometimes be good, because it makes you exert yourself harder and thus improves your performance. Excessive stress – i.e. stress which interferes with normal daily life – can be harmful to your health. People who are under stress may develop habits such as smoking or overeating, which are risk factors for cardiovascular disease.
In addition, researchers increasingly believe that stress may itself be a contributory factor for heart disease. For instance, some studies have found a significant correlation between work stress and the incidence of coronary heart disease; others have revealed a significantly higher level of stress among victims of cardiac death in the final months of their lives compared with people who die of other causes.
It is thus vital that you manage stress in your life well.
Factors you cannot change
Age

A person’s risk of developing cardiovascular disease increases with age.
On average, 80% of those who die of coronary heart disease are aged 65 and above.
Gender

Men
Men generally face a much higher risk of heart disease than women. They also tend to suffer heart attacks earlier in life. However, after women reach menopause, they are just as likely to have heart attacks as their male counterparts of equal age; they are also more likely to die from such cardiac complications than the latter.
Women
Heart disease is often regarded as a “male” disease. Statistics, however, belie this perception.
Cardiovascular disease is the largest single cause of female mortality and accounts for one-third of all deaths among women worldwide, killing more than eight million women annually. A similar trend can be seen in Singapore, where cardiovascular disease is likewise the leading cause of death for women.
Three categories of women – namely, menopausal women, women taking oral contraceptives, and pregnant women – are particularly vulnerable to cardiovascular disease.
Women who have reached menopause have a much higher risk of coronary heart disease and heart attack as compared to those in the pre-menopausal period. This is because of the drop in oestrogen after menopause. Oestrogen is thought to have a protective effect on women’s hearts by lowering their systolic blood pressure and level of LDL (“bad”) cholesterol, while raising level of HDL (“good”) cholesterol.
For women taking oral contraceptives, they may find their blood lipid levels detrimentally affected by the hormones contained in these pills. They are also more likely to have blood clots forming in vital blood vessels. If a woman taking oral contraceptives is also a smoker, her risk of developing cardiac complications would rise, especially once she reaches the age of 35.
Find out more about women and heart disease.
Family History

A family history of stroke or heart disease, especially if it occurred at an early age for the affected family member, is a strong risk factor for cardiovascular illnesses. This is because some of the other contributory factors in this context such as diabetes, high blood pressure, and high LDL cholesterol (or Familial Hypercholesterolemia) may be inherited by children from their parents.
In addition, people often adopt the same lifestyle habits as their parents and siblings do. As a result, the genes and habits that cause us to be sedentary, smoke, to be overweight / obese, or to follow poor diets often tend to cluster in families.
The chances of having a heart attack are higher in people with family members who have a history of heart disease, especially if a first-degree relative has had heart disease before the age of 55 for men and 65 for women.