When The Caregiver Needs Care
Have you heard of caregiver burnout? Caregiver burnout happens when caregivers cannot meet their own physical, emotional and spiritual needs while caring for their loved one. During this process, the caregiver’s attitude may change from positive and caring to negative and unconcerned. Their physical and heart health may also suffer.
Imagine coming home on a sunny day. You grab a bottle in anticipation of quenching your thirst when you realise that the bottle is empty. This analogy represents what it means when a caregiver experiences burnout – the caregiver is empty and has nothing left to give. This feeling of emptiness is not just physical but emotional and mental too.
Caregivers of persons with cardiovascular conditions often experience higher levels of strain and depression and lower social support than noncaregivers. This stress may come from worrying about another heart attack, not knowing what to expect after a loved one’s discharge from the hospital, financial issues and the possibility of losing their loved one.
If you are interested to know how well you are coping as a caregiver, take this self-assessment:
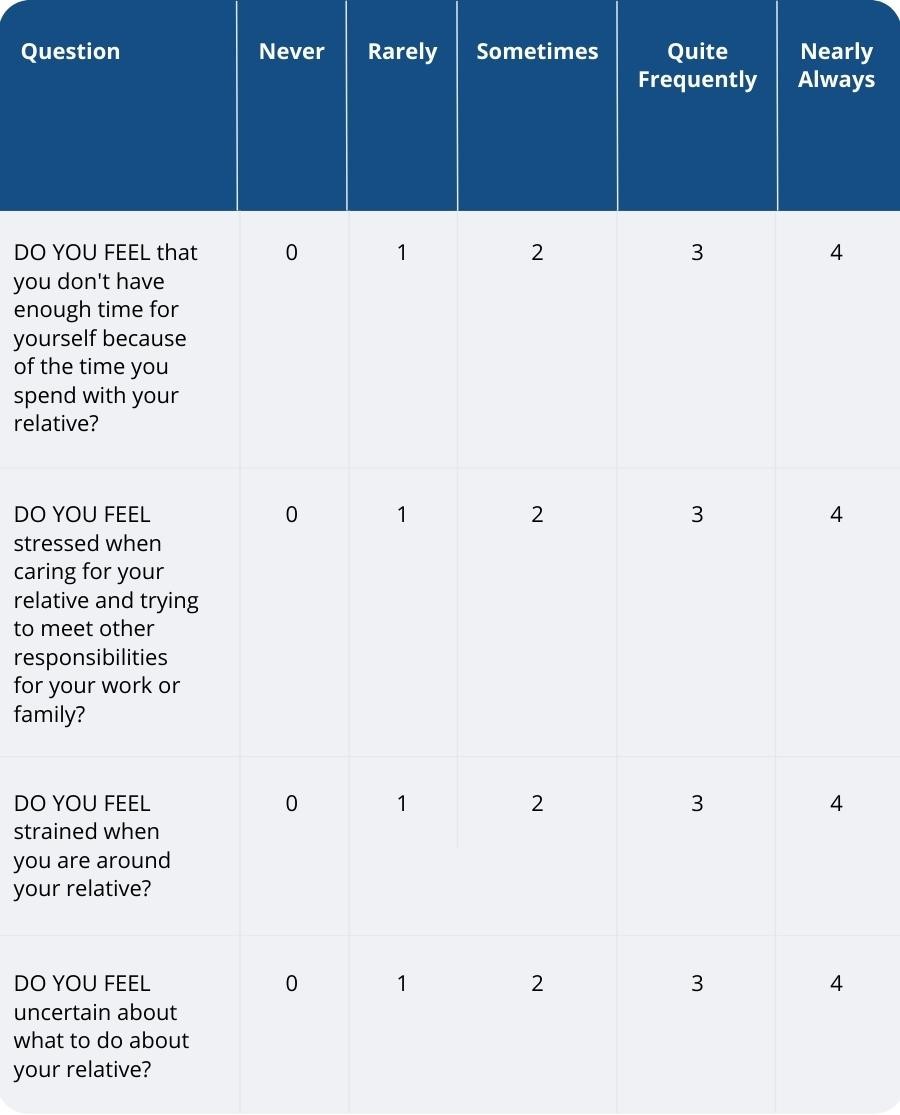
From the Zarit Burden Interview. A score of 8 or higher reflects a high burden and need for additional support.
Signs of caregiver burnout
I once supported a young man who was a caregiver to his mother with a medical condition. He experienced anxiety attacks at the sounds of slight movements in the night and felt urges to check on his mother. His sleep, studies and ability to be an effective caregiver were affected as his physical and mental health suffered.
Burnt-out caregivers may experience the following:
Physical
- Changes in appetite, weight or both
- Difficulty sleeping
- Getting sick more often
- Lack of energy
Social
- Withdrawal from friends and family
- Neglecting responsibilities
- Loss of interest in activities they previously enjoyed
Emotional
- Easily irritable
- Feeling anxious or sad all the time
- Overreacting to minor issues
Spiritual
- Feeling resentful and bitter about life
- Losing a sense of purpose or meaning in life
- Thinking that one is being punished
- Blaming God
Complications of Caregiver Burnout
Chronic stress and negligence in attending to their own health by eating a healthy diet, getting physical activity and treating physical and emotional problems can lead a caregiver to serious health problems that include cardiovascular disease (CVD).
Depression and anxiety
A 2017 meta-analysis linked major depressive disorder to a 72% increased risk for CVD and increases in specific categories of coronary heart disease, cerebrovascular disease, congestive heart failure and CVD-related death. Other meta-analyses have also demonstrated an association between anxiety and a greater risk of cardiac death, incident CVD and stroke.
Obesity
Stress can also affect one’s appetite and influence dietary preferences. People who increase food intake in response to stress report craving foods high in fats and sugar. Energy-dense foods with little physical activity set the stage for the development of overweight and obesity, a risk factor for heart disease and stroke.
Tips for caregivers
Set aside time to refuel
Would you worry if the pilot announces that the plane is out of fuel while you’re en route a long-haul flight? I am sure you will be relieved if the pilot refuels at a stopover before carrying on the journey. Similarly, caregiving is usually a long journey; self-care isn’t a luxury but a necessity.
Caregiving is just one of our many roles, and taking short breaks allows us to manage the other areas of our lives physically, emotionally, socially and spiritually. Allocating time for self-care has proved to decrease caregiver burnout significantly in a study on family caregivers.
Ways to self-care:
Physical care
- Exercise regularly, such as taking walks
- Have a balanced diet
- Go for regular medical check-ups
- Don’t look at your handphone when you can’t sleep at night. Read a book or listen to relaxing music instead.
Emotional care
- Practise self-compassion – relate to yourself in a way that is forgiving, accepting and loving when things are not going their intended way. Allow yourself to feel and cry, and be kind to yourself. Everyone has their limitations on what they can take.
- Find humour to help deal with everyday stressors.
Social care
- Connect and have regular time-out with family and friends.
- Consider joining a caregiver support group. Caregiving can feel like a lonely journey. Hearing from others undergoing similar struggles can reduce that sense of isolation and provide mutual learning and support.
- Ask for help when you need it. It can be for little things like groceries or to watch over your loved one while you take time off.
Spiritual care
- Make time for self-reflection and go for a nature walk.
- Seek religious support or a spiritual advisor if you have a religious belief.
Be equipped and educated
Equip yourself with knowledge about the condition, symptoms and possible progression from your loved one’s medical team by attending caregiver training. Although we cannot predict what will happen, being educated on the progression of the condition helps us to be better prepared.
You can also equip yourself with resources available in the community. Approach a medical social worker to ask about the schemes, programmes and services available for your loved one or yourself. Caregivers who were initially unaware of the support available often struggle alone longer than required. You can check out the one-stop portal by the Agency for Integrated Care which provides digital information and resources for caregivers and care recipients.
Acknowledge and accept
Have meaningful conversations with your loved one about Advance Care Planning and the Lasting Power of Attorney early, as forward planning lessens future financial and care issues. Start by finding out what is important to your loved one. When they are ready, have deeper conversations together with a healthcare professional.
Finally, take time to build positive memories together.
It is important to refuel so that we can refresh our loved ones when they need us.
Caregivers are unsung heroes who provide not for glory or fame but from a sense of duty and without expectations of reciprocation. However, caregivers need care too, even when care recipients are unable to reciprocate that care. On behalf of all care recipients, thank you.
Article is contributed by Mr Roger Tan, Principal Medical Social Worker at the Institute of Mental Health.






